Comprehensive Gynecological Services for Women’s Health
Expert Gynecologic Care for Every Stage of Life
At Marsha E. Gorens, MD, we provide compassionate, personalized gynecological care focused on prevention, wellness, and individualized treatment. Our gynecologic services include routine exams, screenings, contraceptive counseling, and treatment for a wide range of women’s health concerns. With expert guidance and a patient-centered approach, we help women of all ages achieve and maintain optimal reproductive health.
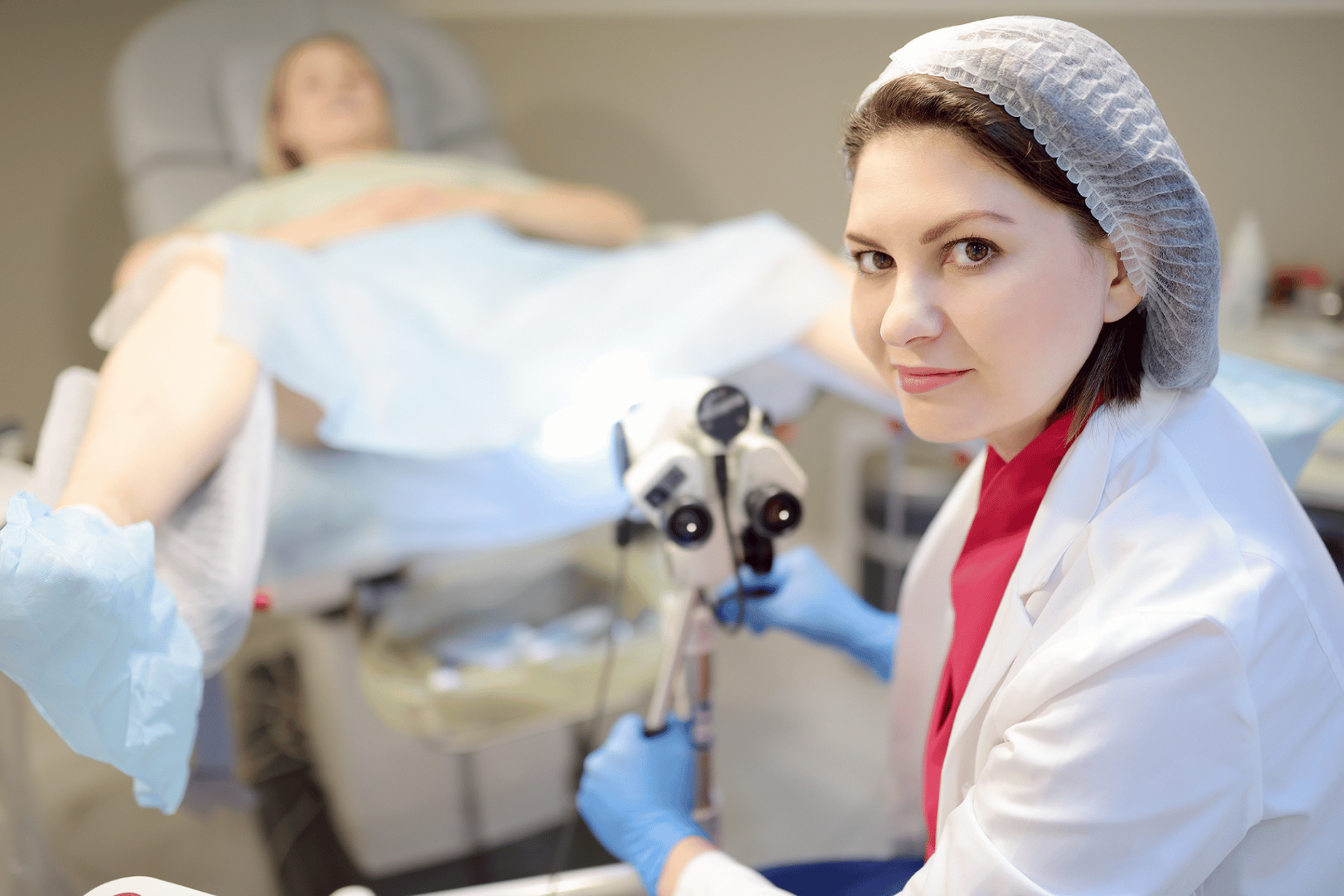
Gynecologist Specialist
Women’s health is about more than routine health exams. It’s about caring for yourself from the inside out. Dr. Marsha E. Gorens is a gynecologist in Near West Side, Chicago who understands the complexity of women’s health care and provides medical treatment in addition to aesthetic procedures. Call Marsha E. Gorens, MD, or schedule an appointment online to learn more about how she can help you reach optimal health.
What is a gynecologist?
A gynecologist is a doctor who specializes in women’s health and the female reproductive system. This field of medicine focuses on providing care and treatments for conditions unique to women and their sexual health such as fertility, incontinence, and hormonal imbalances.
What types of services do gynecologists provide?
A few of the common services provided by gynecologists include cervical cancer and HPV screenings, testing for sexually-transmitted diseases, and contraceptive counseling.
- Cervical cancer and HPV screening
There are many strains of human papillomavirus (HPV), and some can lead to cervical cancer. A Pap smear performed every one to three years, depending on your age, can detect abnormal cells that may lead to cervical cancer.
- Sexually-transmitted diseases (STDs)
Women often have no symptoms with an STD, so they might have an infection without knowing it. When left untreated, STDs can recur and have debilitating effects.
- Contraceptives counseling
Choosing a method of contraception that’s right for you involves several factors. Dr. Gorens can furnish the information you need to make an informed decision.
- Breast cancer screenings
Gynecologists also provide breast cancer screenings. Women over 20 should examine their breasts monthly for signs of pain, swelling, or lumps. If abnormalities are present, you should schedule an appointment with Dr. Gorens. When you reach 40, you need an annual mammogram and clinical exam.
- Excessive menstrual bleeding
Also known as menorrhagia, excessive menstrual bleeding is a condition that involves blood loss and cramps that are so severe that they disrupt your daily activities.
You might have menorrhagia if you pass blood clots that are larger than a quarter, need to double your sanitary protection or have to change your pads or tampons every hour for several hours in a day.
Excessive menstrual bleeding can have a variety of causes, including uterine fibroids and endometriosis. Dr. Gorens gets to the bottom of your issue and recommends appropriate treatment to give you relief from your uncomfortable symptoms.
Are tests and treatments for thyroid disorders included in gynecologic care?
Dr. Gorens helps women manage thyroid disorders as part of an overall wellness plan, and your yearly gynecologic exam is the perfect time to monitor your thyroid blood work. She may also check your hormone levels any time you’re experiencing symptoms that may be related to your thyroid.
If you’re due for an annual gynecologic exam or have a women’s health issue you’d like to discuss with Dr. Gorens, call the office or schedule an appointment online today.

Women's Health
At Marsha E. Gorens, MD, we provide comprehensive women’s health care focused on prevention, education, and personalized treatment. From routine exams and screenings to contraceptive counseling and specialized gynecologic care, our goal is to support your health and well-being at every stage of life.
Adolescent Gynecological Exams
Teenage women have questions about their bodies as they enter adulthood. Some become sexually active at a young age and can expose themselves to the risks of pregnancy and disease. A gynecological exam may seem overwhelming, and they may have concerns about confidentiality. Dr. Gorens treats her younger patients with special care and works hard to earn their trust over time. She strives to be the person they can turn to for confidential, professional advice. Women who have reached the age of 18 should have an annual pelvic exam and Pap smear. If the woman is not sexually active before the age of 18, then a full pelvic exam may not be necessary, but a modified pelvic exam is recommended. An exam for an adolescent includes a medical assessment and private consultation in which all her questions will be answered.
Breast Cancer Screening
Breast Cancer affects one of every eight women at some point in their lives. The cause is not yet fully understood, but detection and prevention methods do exist. Each month, women above the age of 20 should examine their breasts for any sign of pain, swelling, or lumps. If abnormalities are found, they should schedule an appointment with the physician. If no abnormalities are present, a physician exam should be scheduled every 1-3 years. Women past the age of 40 need an annual mammogram and clinical exam. If you are unsure of proper methods for self-examination of the breasts, Dr. Gorens will be happy to educate you as part of a routine examination.
Cervical Cancer and HPV Screening
There are many strains of human papillomavirus (HPV), and some can lead to Cervical cancer. Some strains are transmitted sexually. Routine testing can detect these viruses, and treatment is available. A Pap smear performed every one to three years can detect abnormal cells that may lead to cervical cancer. Women over 30 are at greater risk of developing cervical cancer and should have an HPV DNA test at the same time as the Pap smear to detect many of the HPVs that are associated with developing into cervical cancer. HPVs tend to go away in time, but women should be screened regularly to detect them and reduce the risk of cervical cancer.
Contraceptive Counseling
Choosing a method of contraception that is right for you involves weighing many factors, such as health, convenience, frequency, duration, age, and permanency. Dr. Gorens can furnish the information you need in order to make an informed choice.
www.essure.com
Intrauterine Devices (IUD)
IUDs have few side effects and provide long-term protection against pregnancy. They must be inserted and removed by a trained physician in order to be effective and to avoid complications. The physician must measure the cervix and uterus then insert the device to the proper depth. A removal string remains, but removal must be performed by a physician to prevent serious internal injuries.
Pediatric Gynecological Services
Some young patients may have pelvic pain, vulvovaginitis, congenital malformations, or puberty disorders. They may need a preventive exam or treatment for a gynecologic problem. It is recommended that girls over the age of 13 have preventive examinations and consultations in order to establish a relationship of trust with the doctor. The visit begins with a consultation and evaluation with parent and child both present. If a medical exam is needed, Dr. Gorens is experienced and sensitive in working with patients of this age and will do everything to make sure that the visit is positive for the patient and not traumatic.
Sexually Transmitted Diseases (STDS)
Women usually have no symptoms when infected with a sexually transmitted disease (STD,) so they may be infected without knowing it. Anyone with multiple sexual partners should be tested periodically, even if they are protecting themselves with condoms. Women should ask their partners about any history of STDs and seek testing and treatment if they even suspect they have been infected. Most STDs can be treated effectively, but some have no cure at this time. Gonorrhea, chlamydia and syphilis can be treated with antibiotics. Flare-ups of genital warts can be shortened with antiviral medications. HIV has no known cure, but can be treated effectively. Left untreated, STDs can recur and have debilitating effects, so patients are counseled to practice safe sex and seek testing frequently.

Urinary Incontinence Specialist
Urinary incontinence is an embarrassing problem for many women, but Dr. Marsha E. Gorens can help. With more than 28 years providing health care for women, Dr. Gorens has solutions for urinary leakage and other urinary tract conditions. To learn more about urinary incontinence treatments and gynecological care, call Marsha E. Gorens, MD, in the Near West Side, Chicago area or schedule an appointment online.
What is urinary incontinence?
When you lose control of your bladder or have urinary leakage, you are experiencing incontinence. That's a common problem for women that can be mild or severe.
In some cases, only small amounts of urine may leak when you laugh or sneeze. In other cases, you may have a total loss of bladder control.
There are several types of urinary incontinence. The most common include:
- Urge: a frequent, sudden urge to urinate that makes it difficult to reach the bathroom in time; also called overactive bladder
- Stress: urine leakage from pressure on the abdomen like sneezing, coughing, or running
- Mixed: having both urge and stress urinary incontinence at the same time.
What causes urinary incontinence?
Physical conditions or medical problems can cause urinary incontinence, but it’s not a disease. Women are more prone to having incontinence because of several factors. Some of these include:
- Menopause
- Pregnancy
- Childbirth
- Hysterectomy
- Aging
Pelvic floor disorders, neurological disorders, obstructions, and specific diseases can also cause urinary incontinence. Additionally, urinary incontinence is sometimes a temporary condition caused by urinary tract infections, medications, certain beverages, and even spicy foods or chocolate.
How is incontinence diagnosed and treated?
Dr. Gorens performs a full physical examination and discusses your personal medical history to determine the cause of your urinary incontinence. Depending on your symptoms, she might also recommend additional imaging and bladder function tests.
Your treatment depends on the severity of your condition. Dr. Gorens might recommend:
- Lifestyle changes, like managing your fluid intake
- Physical therapy to strengthen the pelvic floor
- Bladder training to retrain your bladder muscles
- Medications to control muscle spasms and relax the bladder
Dr. Gorens might also suggest treatment that includes products from InControl® Medical. These FDA-cleared devices are designed to noninvasively correct incontinence by strengthening your pelvic floor and relaxing bladder muscles.
Some types of urinary incontinence are also treatable with surgery.
Can urinary incontinence be prevented?
Your chances of developing urinary incontinence increase based on several factors including your family history, weight, and age. However, healthy lifestyle choices can help reduce your risks. Some of these modifications include:
- Healthy weight management
- Pelvic floor exercises
- Eating a fiber-rich diet low in bladder irritants
Don’t let urinary incontinence control your life. Call Marsha E. Gorens, MD, or schedule an appointment online today to learn about the treatment options that are available.
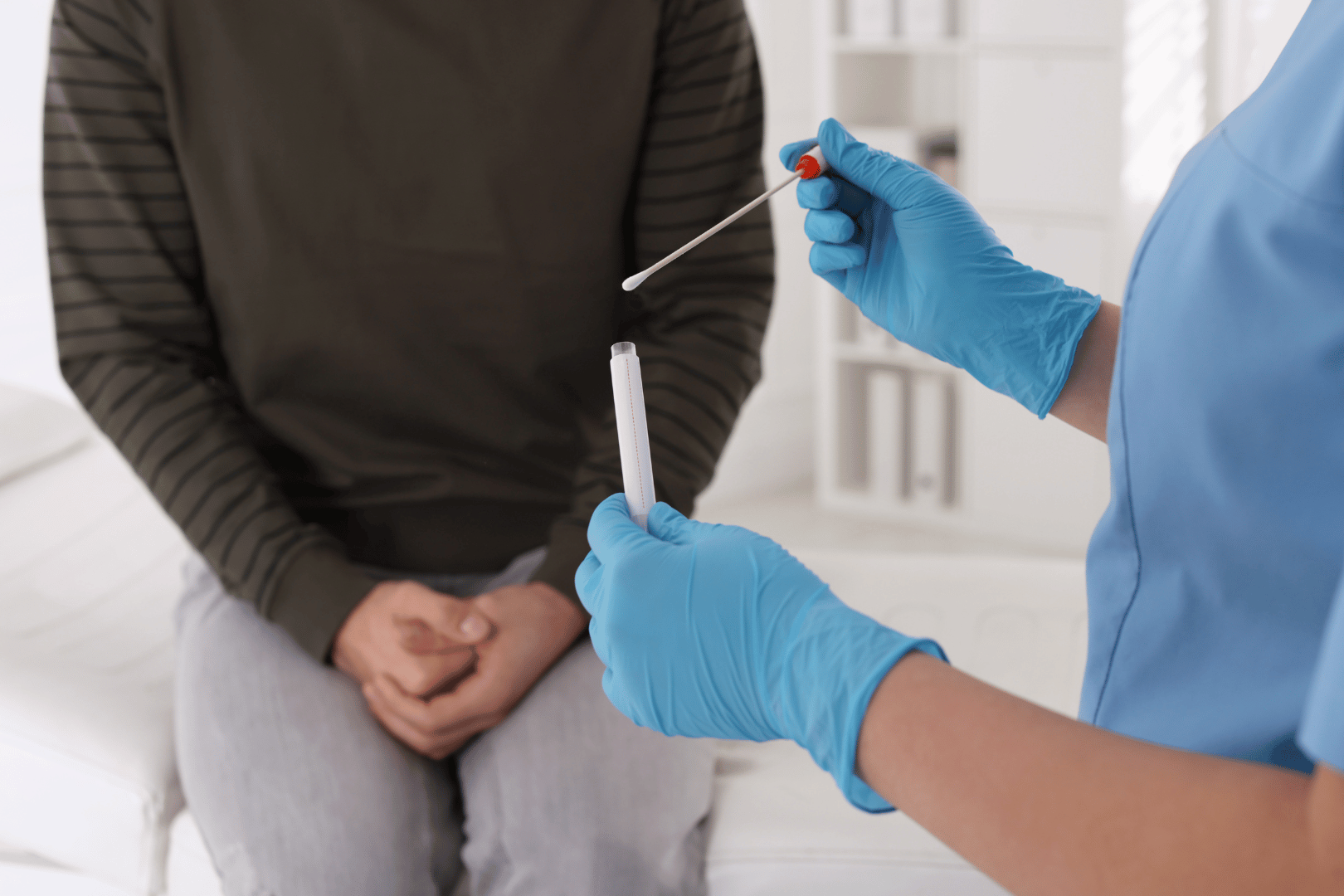
STD Testing Specialist
It can be frightening to think about having a sexually transmitted disease (STD), but they’re incredibly common, and Marsha E. Gorens, MD, can answer your questions and help with treatment. The STD testing process is smooth and easy and usually takes only a few minutes in the Near West Side, Chicago, office. STDs don’t get better without treatment, so don’t wait to find out if you’re infected. Call the office to book an appointment.
What infections does STD testing include?
Sexually transmitted disease or STD testing can check for any kind of infection using blood, urine, swab tests, or tissue samples. Most STDs are bacterial, viral, or parasitic infections, and the most commonly tested for STDs include:
- Chlamydia
- Gonorrhea
- Hepatitis B
- Genital herpes
- HIV
- Human papillomavirus (HPV)
- Syphilis
- Trichomoniasis
Depending on your specific symptoms, your provider can also test for other less common STDs, including chancroid, molluscum contagiosum, and granuloma inguinale.
How often do I need STD testing?
The team recommends a testing schedule appropriate for your situation. In general, you need STD testing if you have symptoms such as:
- New genital discharge
- Genital pain
- Pain during intercourse
- Pelvic area pain
- Fever
- Genital itchiness or burning
- Genital skin changes, including bumps, sores, or other growths
If you have sex with anyone who’s tested positive for an STD, or who has active symptoms of an STD, schedule a test as soon as possible.
The following guidelines also exist for STD testing, regardless of sexual habits:
- Everyone 13-64 needs a minimum of one HIV test during their life
- Women under 25 need annual gonorrhea and chlamydia testing
- Women 25 and older with multiple partners or new partners need annual testing
- All pregnant women need hepatitis B, HIV, and syphilis testing
- At-risk pregnant mothers need gonorrhea and chlamydia testing
- Women who have unprotected sex need annual HIV tests
- Women who share drug needles need HIV tests yearly
Don’t be afraid to discuss your sex life and personal habits with your non-judgemental and caring OB/GYN. This information can help them to personalize your STD testing.
What do my STD testing results mean?
Your provider explains the results and what they mean for you. Generally, a positive test means that you have an active infection requiring treatment.
The specific STD treatment varies with the disease but often includes antibiotics, antivirals, or other types of oral or topical medication. Your provider may also provide counseling on safe-sex practices and how to protect yourself from STDs in the future or decrease the risk of infecting your partner.
An abnormal Pap smear, which often means you have HPV, is a bit different because it may not require immediate treatment. But, your provider may recommend more frequent monitoring so they can remove the HPV cells if they’re likely to become cervical cancer.
Marsha E. Gorens, MD, makes it easy to get your STD testing and treatment in a confidential and supportive environment. Call the office to arrange your STD testing.
More Gynecological Services
Excessive Menstrual Bleeding
Women who experience excessive menstrual bleeding may have tried a variety of treatments without success. They may not be appropriate candidates for hysterectomy or may not wish to undergo that procedure. These patients may consider Endometrial Ablation, an outpatient procedure in which the uterine lining is removed using freezing, electricity, microwave, or heat ablation techniques. The endometrium is removed, leaving the ovaries intact. As the endometrium heals, scar tissue forms and prevents future bleeding. Recovery time is a few days to a few weeks. This procedure is not for women who wish to become pregnant or have a history of cancer or pre-cancer of the uterus.
Fibroid Tumors, Endometriosis Genital Prolapse
Patients with Fibroid Tumors, Endometriosis Genital Prolapse or excessive bleeding may need to have a Hysterectomy, which involves removal of the uterus and sometimes the ovaries and fallopian tubes. A less-extreme procedure called Laparoscopic Supracervical Hysterectomy (LSH)involves removal of the uterus through a small abdominal incision using a laparoscope to allow the surgeon to view the internal area. Traditional abdominal surgery may be avoided altogether with a Laparoscopic-Assisted Vaginal Hysterectomy (LAVH). In this procedure, a small incision in the navel allows the insertion of a laparoscopic device to enable the surgeon to view the internal organs. Surgical access through the vagina allows the surgeon to make the incision needed to remove the uterus. Post-operative recovery is much shorter than that required by traditional abdominal surgery.
Abnormal Cells
If during a routine gynecological exam abnormal cells are found on the surface of the cervix, the doctor will perform a Colposcopy and if the report confirms an abnormality shemay recommend a Loop Electrosurgical Excision Procedure (LEEP). This outpatient procedure may be performed in the doctor's office with local anesthetic in approximately half an hour. Abnormal tissue is excised to prevent the development of cancer of the cervix. Samples are tested to determine possible causes of abnormality. The patient may experience mild discomfort but same-day recovery is typical, and side effects are rare.
Fibroid Tumors
If the patient is found to have non-cancerous tumors of the uterus, she may choose to have a hysterectomy if she no longer has a desire to bear children. For women who plan to have children or who wish to keep their uterus, the physician may recommend a Myomectomy to surgically remove fibroid tumors and repair the uterus. Depending on the type and size of the fibroids, the physician may recommend one of the following procedures.
- Abdominal myomectomy, involving an incision to remove the problem tissue, brief hospitalization, and recovery in 4 to 6 weeks.
- Hysteroscopic myomectomy, in which a small device called a resectoscope enters through the vagina to remove the fibroid tissue.
- Laparoscopic myomectomy, where a small incision allows the surgeon to view the pelvic region with tiny camera and excise the fibroid tissue. Following this hospital procedure, the patient is usually released the same day, and there is a brief recovery period of a few days.
Pelvic Organ Prolapse
When abdominal muscles are weakened after childbirth or surgery, an organ may drop from its normal location. The patient feels pressure in the area of the vagina and may experience incontinence. The condition is often painful, but is not considered a serious health problem and may correct itself over time. If symptoms do not go away, the physician may recommend a Pelvic Prolapse Repair Surgery on the affected organs. Proper treatment can prevent future recurrence.
Permanent Sterilzation
Women who wish to end the possibility of pregnancy may choose to become sterilized using an Essure Tubal Ligation. This procedure may be performed in the doctor's office and involves inserting small flexible micro-inserts™ into the fallopian tubes, reached through the vagina, cervix, and uterus. Most patients can return to work and normal activities the same day or following day. Birth control methods must continue and may be stopped following an examination and verification test three months after the procedure is performed. Women still have the option of having a more invasive laparoscopic procedure to perform a tubal sterilization but they need to be informed of a less invasive procedure that does not rquire incisions or general anesthesia.